British Transport Police, Metropolitan Police and City of London Police reshaping police mental health crisis response
30 April 2026

Across England and Wales, some of the most recognisable names in policing are taking a more deliberate, forward-looking approach to one of the most complex areas of modern service delivery.
British Transport Police, Metropolitan Police Service and City of London Police are each building on existing approaches to improve how mental health incidents are managed in practice. This includes strengthening how information is accessed and shared with police colleagues and healthcare partners, improving the consistency of decision-making, and creating a clearer, real-time understanding of what is happening across mental health crisis pathways.
This reflects a broader shift in how forces are thinking about their role within a multi-agency system. Mental health response is operationally demanding, often time critical, and heavily dependent on the availability and quality of information at the point decisions are made. In this context, improvement is less about replacing existing processes and more about making them more efficient, more coordinated and more productive across organisational boundaries.
This shift is also unfolding alongside the implementation of Right Care, Right Person, which aims to ensure that individuals with health or social care needs are supported by the most appropriate professional, rather than police being the default responder. While this has the potential to improve outcomes and release police time back into core activity, it also increases the importance of how responsibility is shared across the system. A growing number of Prevention of Future Deaths reports are beginning to highlight the risks where this transition is not fully supported, particularly where alternative services are not yet able to respond at the required pace or scale. In that context, digital infrastructure becomes critical to maintaining visibility and continuity across the pathway, helping to ensure that as responsibilities shift, individuals do not fall between the gaps.
Over the past 12 months, these forces have focused on embedding approaches that support this, with an increasing emphasis on visibility, coordination and consistent decision-making. What is emerging is not simply process improvement, but the early shape of a more connected and manageable model of crisis response.
If you’d like to hear more about how Thalamos could help your police force then please book a call with our team.
From intent to impact: what this looks like in practice

That shift towards more modern, data-informed ways of working is already translating into measurable operational change.
British Transport Police (BTP) provides one of the clearest early examples of what this looks like when applied at scale. Operating across England, Scotland and Wales, and frequently interfacing with multiple health systems in a single day, BTP sits at a particularly complex intersection of policing and mental health response. The challenge has historically been less about intent and more about the difficulty of managing a fragmented pathway without real-time visibility.
What has changed over the past year is the ability to see, understand and act on that pathway as it unfolds.
Following national rollout in July 2025, digital workflows are now embedded across the force, supporting the recording and sharing of Section 136 activity in real time. Within six months, this approach reached 95% officer adoption across a national force, demonstrating not just implementation, but operational acceptance.
That adoption has translated directly into operational impact. The average time officers spend at health-based places of safety has reduced from 219 minutes to 79 minutes per incident, a 63% decrease. This represents a meaningful return of officer time to core policing activity, improving both capacity and responsiveness across the network. Over six months, this equated to approximately £45,000 in efficiency savings, or over £90,000 when annualised.
At the same time, the quality and consistency of decision-making is beginning to improve. Structured workflows support earlier engagement with healthcare professionals, contributing to an increase in consultation prior to detention, while handover performance has improved against the four-hour standard.

The more fundamental shift, however, sits beneath these metrics. For the first time, BTP has access to real-time, structured data across its mental health pathway. Rather than relying on delayed, inconsistent reporting, supervisors and operational leads can see where delays are occurring, how practice varies across locations, and where intervention is required while incidents are still live.
This moves mental health response from something that is reviewed after the fact to something that can be actively managed in the moment. It also begins to reshape collaboration with health partners. Where shared information is accessed and used, handovers become more predictable, communication improves, and the pathway functions with greater alignment across organisational boundaries.
Building on foundations: strengthening control in the Metropolitan Police

If British Transport Police demonstrates what becomes possible when visibility is established, the Metropolitan Police Service (MPS) reflects the next stage of that journey, where existing capability is actively refined and extended.
In London, the scale and complexity of demand place additional pressure on how mental health incidents are managed. A dense network of NHS providers, local authorities and emergency services means that coordination and consistency are critical to effective response. In this environment, digital capability is not static. It needs to evolve alongside operational reality.
The MPS move to a more advanced version of its digital mental health capability, having been a Thalamos user since 2022, reflects a clear recognition of this. Rather than treating digitisation as a one-off implementation, the focus has shifted towards how that capability can be deepened over time. This includes strengthening operational oversight through supervisor dashboards that highlight incidents approaching critical thresholds, improving how information can be shared in practice through more flexible sharing mechanisms, and introducing structured prompts that ensure incidents are actively updated as they unfold. At the same time, workflows have been redesigned to better reflect operational reality, allowing both police and NHS users to input and update information based on shared understanding in the moment, rather than relying on sequential input from each organisation. This reduces delays, improves data completeness, and enables incidents to progress more efficiently.
This is increasingly reflected in how the Metropolitan Police Service is using data within the pathway to inform operational practice. Improvements are not confined to better visibility at the point of detention, but extend into how incidents are tracked, shared and progressed across organisations. Enhanced handover processes allow information to move more reliably between police and NHS teams, while structured activity logs provide a clearer, shared account of what is happening during an incident, including the rationale for ongoing police presence. Integration with NHS records enables information captured by officers to be carried forward into clinical systems, reducing duplication and supporting continuity of care. At the same time, outcome tracking begins to close the loop on the pathway, allowing forces to understand not just how incidents are managed, but what happens next. Taken together, this reflects a more deliberate use of data, not simply to observe the pathway, but to shape how it functions in practice.
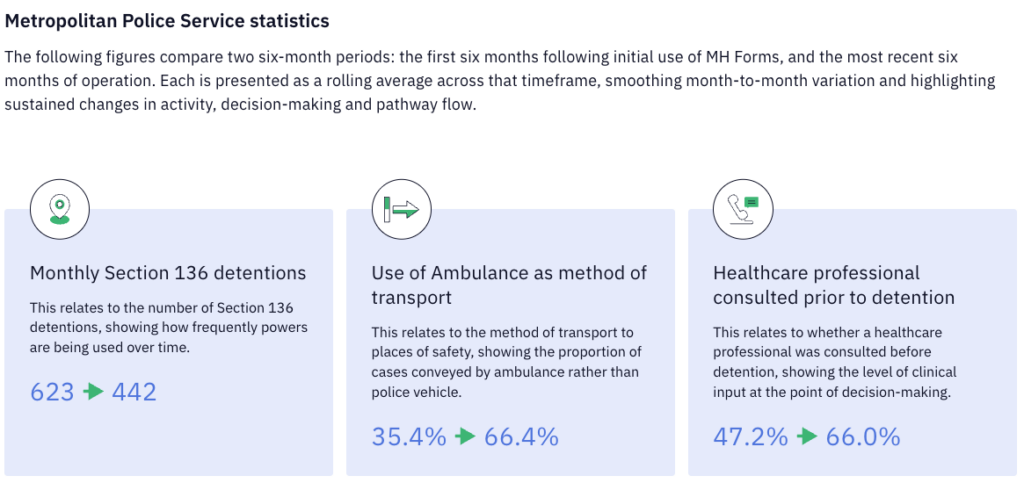
Over time, the impact of the MPS’ combined approach is beginning to show clearly in the data. Comparing the first six months of use to the most recent six-month period, the Metropolitan Police Service has seen a reduction of almost 30% in average monthly Section 136 detentions, alongside a marked shift in how individuals are conveyed to places of safety. Ambulance usage has increased from 35% to 66%, indicating a move towards more clinically led transport decisions, while healthcare professional consultation prior to detention has risen from 47% to 66%. Taken together, these changes point to a more informed, better coordinated approach to decision-making, where clinical input is more consistently embedded and the use of police-led interventions becomes more targeted and proportionate.
This progression is particularly important in the context of ongoing policy and system change. Developments such as Right Care, Right Person, alongside sustained pressure on health services, continue to reshape how demand presents and how it needs to be managed. Systems that cannot adapt risk becoming a constraint rather than an enabler. It also enables a more continuous, end-to-end view of the pathway, with NHS teams able to carry forward and build on the initial police record as the individual moves through assessment and care.
By investing in the next iteration of its approach, the Metropolitan Police Service is positioning itself to respond to that shifting landscape with greater confidence. The emphasis is no longer solely on digitising existing processes, but on gaining tighter operational control of how those processes function in real time.
For other forces, this illustrates that the value of modernisation is not confined to initial implementation. It increases as organisations refine their approach, respond to emerging pressures, and build a more complete understanding of the pathways they are managing.
Strengthening the system: City of London Police and the power of alignment

If the experience of BTP and MPS highlights the importance of visibility and progression, the recent go-live of City of London Police (CoLP) brings into focus the role of alignment across the wider system.
For (CoLP), modernisation is not solely an internal exercise. It is about operating more effectively within a landscape where incidents frequently cross organisational boundaries, and where outcomes depend on how well information is shared between services.
Adopting a consistent, structured approach to managing mental health incidents reduces variation in how those incidents are handled. It supports more reliable decision-making, particularly in high-pressure scenarios, and enables more predictable and coordinated handovers between police and health partners.
This becomes increasingly important in environments like London, where multiple forces and NHS organisations are often involved in the same pathway. Without a shared framework, each interaction introduces the potential for delay, duplication or miscommunication. With one in place, those interactions become more streamlined, more transparent, and easier to manage.
The CoLP go-live therefore represents part of a broader shift towards a more connected model of crisis response. As more forces align around a common approach, the benefits extend beyond individual organisations.
Over time, this alignment enables a more consistent dataset to emerge across multiple forces. This creates the foundation for a clearer understanding of how mental health demand presents across regions, where pressures are most acute, and how different parts of the pathway are performing. It also strengthens the ability of policing to engage with health partners and commissioners from a position of evidence.
A new baseline for mental health crisis response
Taken together, the approaches being adopted by British Transport Police, the Metropolitan Police Service and City of London Police point towards a new baseline for mental health crisis response.
This is a model that is more visible, more consistent, and more connected. It reduces the administrative burden on frontline officers while improving the quality of information available at the point of decision-making. It also enables forces to move beyond reacting to individual incidents, towards actively managing the pathways that sit behind them.
The challenges within mental health crisis care remain significant. Demand continues to grow, system capacity is uneven, and responsibility is shared across multiple organisations. What is now emerging, however, is a more practical foundation for addressing those challenges.
For the first time, forces are beginning to put in place the infrastructure needed to understand what is happening across these pathways in real time, and to act on that understanding in a consistent and informed way. As more organisations adopt and build on this approach, the gap between intention and operational reality becomes easier to close.
For police forces that have not yet taken this step, the question is becoming increasingly difficult to ignore. Not whether improvement is needed, but whether existing ways of working provide the visibility, coordination and control required to deliver it.
For forces looking to take a more structured and informed approach to mental health crisis response, this shift is already underway.
If you’d like to hear more about how Thalamos could help your police force then please book a call with our team.


